Apr 05, 2015
LED therapy for neurorehabilitation
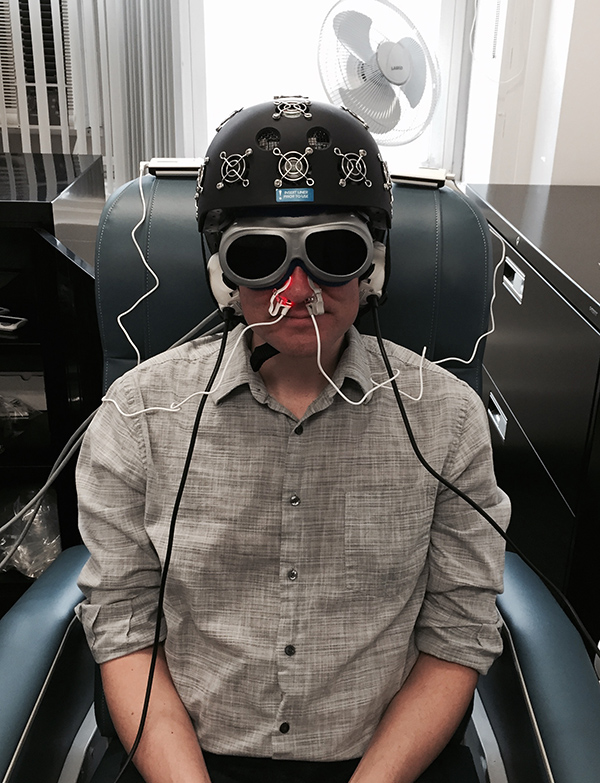
A staffer in Dr. Margaret Naeser’s lab demonstrates the equipment built especially for the research: an LED helmet (Photomedex), intranasal diodes (Vielight), and LED cluster heads placed on the ears (MedX Health). The real and sham devices look identical. Goggles are worn to block out the red light to avoid experimental artifacts. The near-infrared light is beyond the visible spectrum and cannot be seen. (credit: Naeser lab)
Researchers at the VA Boston Healthcare System are testing the effects of light therapy on brain function in the Veterans with Gulf War Illness study.
Veterans in the study wear a helmet lined with light-emitting diodes that apply red and near-infrared light to the scalp. They also have diodes placed in their nostrils, to deliver photons to the deeper parts of the brain.
The light is painless and generates no heat. A treatment takes about 30 minutes.
The therapy, though still considered “investigational” and not covered by most health insurance plans, is already used by some alternative medicine practitioners to treat wounds and pain.
The light from the diodes has been shown to boost the output of nitric oxide near where the LEDs are placed, which improves blood flow in that location.
“We are applying a technology that’s been around for a while,” says lead investigator Dr. Margaret Naeser, “but it’s always been used on the body, for wound healing and to treat muscle aches and pains, and joint problems. We’re starting to use it on the brain.”
Naeser is a research linguist and speech pathologist for the Boston VA, and a research professor of neurology at Boston University School of Medicine (BUSM).
How LED therapy works
The LED therapy increases blood flow in the brain, as shown on MRI scans. It also appears to have an effect on damaged brain cells, specifically on their mitochondria. These are bean-shaped subunits within the cell that put out energy in the form of a chemical known as ATP. The red (600 nm) and NIR (800–900nm) wavelengths penetrate through the scalp and skull by about 1 cm to reach brain cells and spur the mitochondria to produce more ATP. That can mean clearer, sharper thinking, says Naeser.
Nitric oxide is also released and diffused outside the cell wall, promoting local vasodilation and increased blood flow.
Naeser says brain damage caused by explosions, or exposure to pesticides or other neurotoxins — such as in the Gulf War — could impair the mitochondria in cells. She believes light therapy can be a valuable adjunct to standard cognitive rehabilitation, which typically involves “exercising” the brain in various ways to take advantage of brain plasticity and forge new neural networks.
“The light-emitting diodes add something beyond what’s currently available with cognitive rehabilitation therapy,” says Naeser. “That’s a very important therapy, but patients can go only so far with it. And in fact, most of the traumatic brain injury and PTSD cases that we’ve helped so far with LEDs on the head have been through cognitive rehabilitation therapy. These people still showed additional progress after the LED treatments. It’s likely a combination of both methods would produce the best results.”
Results published from 11 TBI patients
The LED approach has its skeptics, but Naeser’s group has already published some encouraging results in the peer-reviewed scientific literature.
Last June in the Journal of Neurotrauma, they reported in an open-access paper, the outcomes of LED therapy in 11 patients with chronic TBI, ranging in age from 26 to 62. Most of the injuries occurred in car accidents or on the athletic field. One was a battlefield injury, from an improvised explosive device (IED).
Neuropsychological testing before the therapy and at several points thereafter showed gains in areas such as executive function, verbal learning, and memory. The study volunteers also reported better sleep and fewer PTSD symptoms.
The study authors concluded that the pilot results warranted a randomized, placebo-controlled trial — the gold standard in medical research.
That’s happening now, thanks to VA support. One trial, already underway, aims to enroll 160 Gulf War veterans. Half the veterans will get the real LED therapy for 15 sessions, while the others will get a mock version, using sham lights.
Then the groups will switch, so all the volunteers will end up getting the real therapy, although they won’t know at which point they received it. After each Veteran’s last real or sham treatment, he or she will undergo tests of brain function.
Naeser points out that “because this is a blinded, controlled study, neither the participant nor the assistant applying the LED helmet and the intranasal diodes is aware whether the LEDs are real or sham — they both wear goggles that block out the red LED light.” The near-infrared light is invisible.
Upcoming trials
Other trials of the LED therapy are getting underway:
- Later this year, a trial will launch for Veterans age 18 to 55 who have both traumatic brain injury (TBI) and post-traumatic stress disorder, a common combination in recent war Veterans. The VA-funded study will be led by Naeser’s colleague Dr. Jeffrey Knight, a psychologist with VA’s National Center for PTSD and an assistant professor of psychiatry at BUSM.
- Dr. Yelena Bogdanova, a clinical psychologist with VA and assistant professor of psychiatry at BUSM, will lead a VA-funded trial looking at the impact of LED therapy on sleep and cognition in Veterans with blast TBI.
- Naeser is collaborating on an Army study testing LED therapy, delivered via the helmets and the nose diodes, for active-duty soldiers with blast TBI. The study, funded by the Army’s Advanced Medical Technology Initiative, will also test the feasibility and effectiveness of using only the nasal LED devices — and not the helmets — as an at-home, self-administered treatment. The study leader is Dr. Carole Palumbo, an investigator with VA and the Army Research Institute of Environmental Medicine, and an associate professor of neurology at BUSM.
Naeser hopes the work will validate LED therapy as a viable treatment for veterans and others with brain difficulties. She also foresees potential for conditions such as depression, stroke, dementia, and even autism.
According to sources cited by the authors, i is estimated that there are 5,300,000 Americans living with TBI-related disabilities. The annual economic cost is estimated to be between $60 and $76.5 billion. It is estimated that 15–40% of soldiers returning from Iraq and Afghanistan as part of Operation Enduring Freedom/Operation Iraqi Freedom (OEF/OIF) report at least one TBI. And within the past 10 years, the diagnosis of concussion in high school sports has increased annually by 16.5%.
The research was supported by U.S. Department of Veterans Affairs. National Institutes of Health, American Medical Society for Sports Medicine, and American College of Sports Medicine-American Medical Society for Sports Medicine Foundation.
22:59 Posted in Brain training & cognitive enhancement, Cybertherapy | Permalink | Comments (0)







The comments are closed.